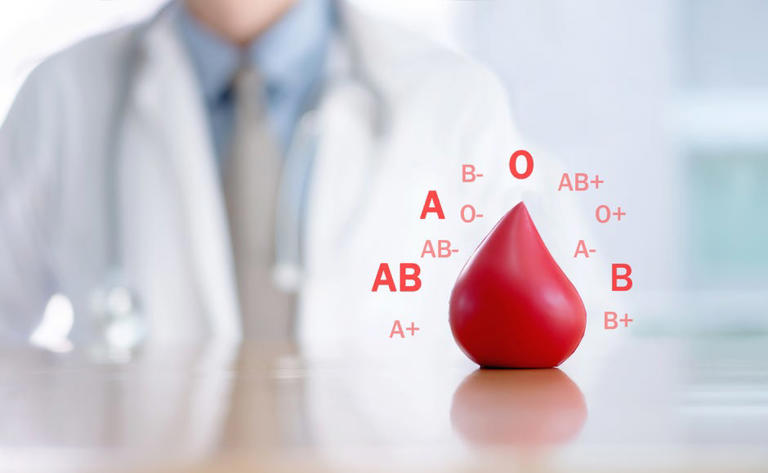
Your blood type is more than just a letter and a symbol on a medical chart; it’s a fundamental part of your biological identity. Think of it as a unique ID card for your red blood cells. Knowing this code is crucial in medical emergencies, during pregnancy, and for organ transplants, ensuring that your body accepts what it’s given without a dangerous reaction.
At its core, your blood type is determined by the presence or absence of specific markers, called antigens, on the surface of your red blood cells. The combination of two key systems—ABO and Rh—gives us the eight common blood types we know.
The Eight Common Blood Types
The four main groups are A, B, AB, and O. These are then further defined by the Rhesus (Rh) factor, a specific protein that can be present (+) or absent (-). This creates the eight possible types:
-
A-Positive (A+)
-
A-Negative (A-)
-
B-Positive (B+)
-
B-Negative (B-)
-
O-Positive (O+)
-
O-Negative (O-)
-
AB-Positive (AB+)
-
AB-Negative (AB-)
How Blood Typing Works: The ABO and Rh Systems
The ABO System: The Letter
This system is all about the A and B antigens.
-
Type A: Has A antigens and makes anti-B antibodies. (It accepts A, attacks B).
-
Type B: Has B antigens and makes anti-A antibodies. (It accepts B, attacks A).
-
Type AB: Has both A and B antigens and makes neither antibody. It’s the universal acceptor for ABO types.
-
Type O: Has no A or B antigens and makes both anti-A and anti-B antibodies. It’s the universal donor for ABO types because it has nothing for other blood types to attack.
The Rh System: The + or –
This is a separate antigen, the Rhesus factor.
-
Rh-Positive (+): The Rh factor is present.
-
Rh-Negative (-): The Rh factor is absent. Rh-negative blood will produce antibodies if exposed to Rh-positive blood.
How to Find Out Your Blood Type
Curious about your own type? You have a few options:
-
Ask Your Doctor: A simple blood draw at your healthcare provider’s office is the most accurate method.
-
Donate Blood: This is a fantastic and free way to find out. Blood banks test every donation and will typically provide you with your blood type information afterward.
-
At-Home Test Kits: Available online or at pharmacies, these kits are generally reliable for basic ABO and Rh typing, though a clinical test is considered the gold standard.
Why Compatibility is Critical: The Universal Donor and Recipient
Mixing incompatible blood types can trigger a severe immune response, as the recipient’s antibodies attack the “foreign” donor blood. This is why matching is essential.
Here’s a quick guide to who can donate to whom:
| Donor Blood Type | Can Donate To… |
|---|---|
| O- | Everyone (The Universal Donor) |
| O+ | O+, A+, B+, AB+ |
| A- | A-, A+, AB-, AB+ |
| A+ | A+, AB+ |
| B- | B-, B+, AB-, AB+ |
| B+ | B+, AB+ |
| AB- | AB-, AB+ |
| AB+ | AB+ (The Universal Recipient) |
Key Takeaways:
-
O-negative is the universal donor. In a trauma situation where there’s no time to test a patient’s blood type, O-negative is used because it’s safe for everyone.
-
AB-positive is the universal recipient. Because it has all the antigens, it doesn’t have antibodies to attack A, B, or Rh-positive blood.
A Snapshot of Rarity
Some blood types are much more common than others. In the U.S.:
-
Most Common: O+ (38% of the population)
-
Rarest Common Type: AB- (less than 1%)
-
The Rarest of All: There is an extremely rare type called Rh-null, or “golden blood.” Lacking all Rh antigens, it’s incredibly valuable as a universal donor for others with rare Rh-negative types, but it’s exceptionally difficult to find a match for someone with Rh-null blood themselves.
The Genetics of Blood Type
You inherit your blood type from your parents, much like your eye color. Each parent contributes one allele (a version of the gene) for ABO and one for Rh.
-
A and B alleles are dominant; O is recessive.
-
Rh-positive is dominant; Rh-negative is recessive.
For example, two O-type parents can only have O-type children. An AO parent (who presents as type A) and a BO parent (who presents as type B) could have a child with type A, B, AB, or O blood.
Frequently Asked Questions (FAQ)
Q: Can my blood type change over my lifetime?
A: Generally, no. Your blood type is genetically determined and remains constant. The only exception is in rare medical cases, such as a bone marrow transplant, where your blood-forming system is replaced by a donor’s.
Q: Do certain blood types have a higher risk for specific diseases?
A: Some research has suggested correlations. For instance, Type O may have a slightly lower risk of heart attacks and blood clots, while non-O types might be more susceptible. Type A has been studied for a potential link to higher stomach cancer risk. However, these are minor risk factors; lifestyle choices like diet and exercise have a far greater impact on your overall health.
Q: I’m Rh-negative and pregnant. What does that mean?
A: This is very important. If an Rh-negative mother carries an Rh-positive baby, her body might develop antibodies that can attack the baby’s red blood cells in a subsequent pregnancy (a condition called Rh incompatibility). Fortunately, this is easily prevented with a simple injection called Rh immunoglobulin (RhoGAM) during and after pregnancy.
Q: Is there such a thing as a “best” blood type to have?
A: Not really. Each has its pros and cons. While O-negative is a lifesaver for others in emergencies, a person with O-negative can only receive O-negative blood. AB-positive individuals can receive from anyone but can only donate to other AB-positive individuals. It’s a biological trade-off!
Q: Where can I get my blood type tested for free?
A: Donating blood is the most common way to get a free and accurate test. Your local blood bank or organizations like the American Red Cross will provide this information to you after you donate.